Healthcare organizations are under increasing pressure to modernize their technology stack while improving outcomes, reducing costs, and performing in value-based care environments.
At some point, every organization faces the same question: Should we build custom software, or buy an off-the-shelf solution?
In reality, this is the wrong question.
Based on our experience working with health plans and provider organizations, the most successful organizations are not choosing between build or buy, they are designing integrated, hybrid ecosystems that combine both.
The Reality: Healthcare Technology Is an Ecosystem
Most healthcare organizations already operate within a complex landscape that includes:
· Core systems (EHR, claims, enrollment, UM/CM platforms)
· Point solutions (coding tools, analytics platforms, engagement solutions)
· Manual workflows bridging gaps between systems
The challenge is not selecting a single system, it’s connecting and orchestrating these components to support real-world workflows.
This becomes even more critical in value-based care, where performance depends on:
• Accurate risk adjustment (RAF)
• Timely care gap closure
• Coordinated care management
• Real-time operational visibility
No single “built” or “bought” system solves all of these requirements.
The Limitations of the “Buy” Approach
Off-the-shelf healthcare software plays an important role, particularly for systems of record like EHRs and claims platforms.
Where It Works:
• Faster implementation timelines
• Lower upfront investment|
• Standardized functionality for common use cases
• Built-in compliance frameworks
Where It Breaks Down:
• Workflow misalignment: Organizations adapt to the software instead of the software adapting to them
• Limited flexibility: Vendor roadmaps dictate innovation
• Integration challenges: Connecting disparate systems often introduces latency and complexity
• Scaling costs: Per-user or PMPM pricing models increase as organizations grow
In value-based care environments, these limitations often result in fragmented workflows and missed performance opportunities.
The Challenges of Full Custom Build
Custom development is often viewed as a way to overcome these limitations, but it introduces its own risks.
Where It Works:
• Highly differentiated workflows
• Unique care delivery models
• Competitive IP development
Where It Falls Short:
• High upfront investment and long timelines
• Ongoing maintenance burden and technical debt
• Regulatory and compliance complexity
• Difficulty keeping pace with evolving healthcare requirements
In our experience, fully custom platforms are rarely the most efficient or scalable solution particularly when organizations already have significant system investments in place.
A Better Approach: The Hybrid (Overlay) Model
Leading healthcare organizations are increasingly adopting a hybrid approach, combining the strengths of both build and buy strategies.
This model consists of three layers:
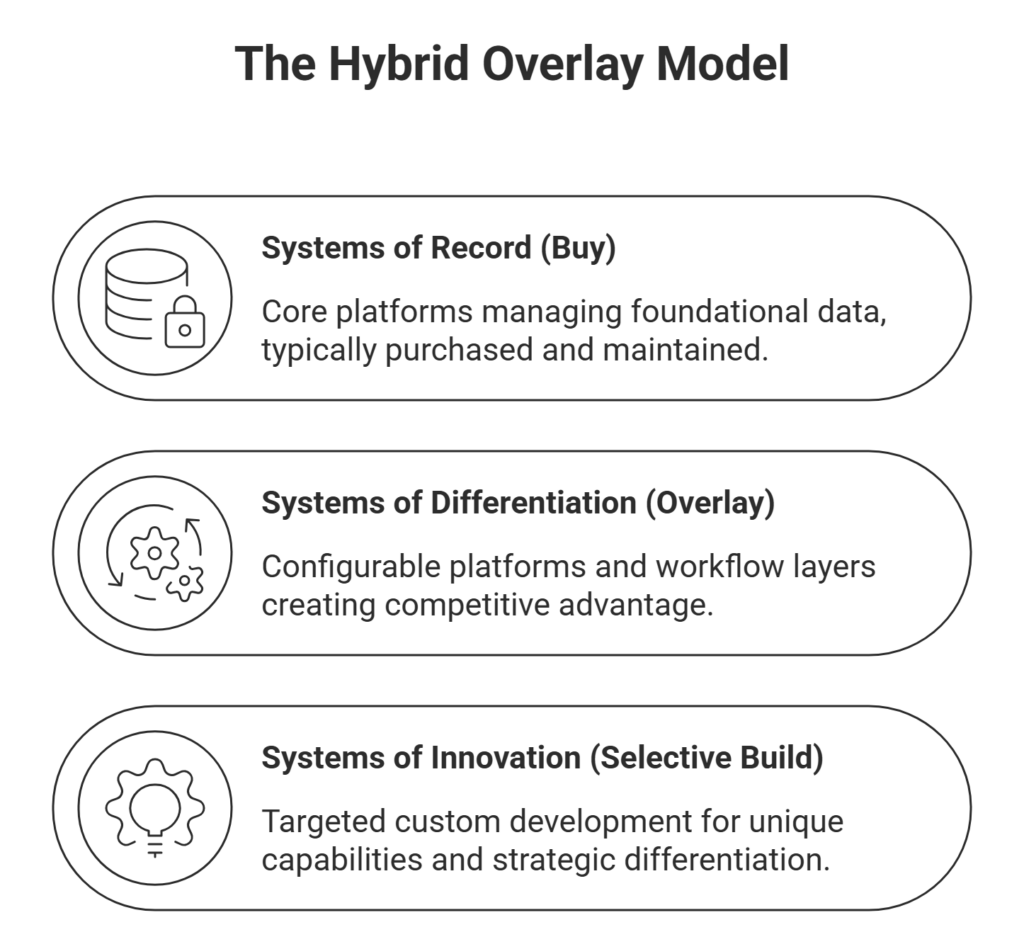
1. Systems of Record (Buy)
Core platforms that manage foundational data:
• EHR
• Claims and enrollment systems
• Billing and finance
These systems are typically best purchased and maintained as enterprise platforms.
2. Systems of Differentiation (Overlay / Configure)
This is where organizations create competitive advantage.
Examples include:
• Risk adjustment workflows
• Care management orchestration
• Care gap closure workflows
• Provider engagement and outreach
Instead of building from scratch, organizations leverage configurable platforms and workflow layers to:
• Integrate across systems
• Enable real-time decision-making
• Adapt to evolving operational needs
3. Systems of Innovation (Selective Build)
Targeted custom development is reserved for:
• Unique capabilities
• Proprietary models
• Strategic differentiation
This ensures organizations invest in building only where it truly creates value.
Why the Hybrid Approach Works:
Organizations that adopt this model can:
Accelerate Time to Value:
By leveraging existing systems and configurable platforms, implementation timelines can be reduced by 20–40% compared to full custom builds.
Improve Operational Efficiency:
Integrating workflows across systems reduces manual effort and fragmentation often improving efficiency by 30–50%.
Enhance Value-Based Care Performance:
By embedding intelligence into workflows, organizations can:
• Improve RAF accuracy and recapture rates
• Increase care gap closure
• Reduce avoidable utilization and readmissions
Reduce Total Cost of Ownership:
Avoiding large-scale custom builds while minimizing vendor lock-in leads to more sustainable long-term cost structures.
The Missing Link: Integration and Workflow Orchestration
In healthcare, the true complexity is not in individual systems, it’s in how they work together.
Fragmented integrations, delayed data, and disconnected workflows create:
• Gaps in care delivery
• Missed risk adjustment opportunities
• Inefficient operations
A modern approach requires:
• API-first integration (FHIR, HL7)
• Near real-time data ingestion
• Unified longitudinal patient records
• Workflow orchestration across systems
This is where many organizations struggle and where the hybrid model delivers the most value.
Incuvio’s Approach: Designing for Real-World Execution
At Incuvio, we help healthcare organizations move beyond the build vs buy dilemma by designing scalable, integrated technology strategies.
Our approach focuses on:
• Leveraging existing system investments rather than replacing them
• Integrating data across sources to create a trusted, unified view
• Embedding intelligence into workflows to drive real-time action
• Enabling flexibility to adapt as value-based care requirements evolve
This allows organizations to transition from:
• Fragmented systems → Connected ecosystems
• Reactive operations → Proactive, data-driven workflows
• Missed opportunities → Measurable performance improvement
Looking Ahead
Healthcare organizations that succeed in the next phase of transformation will not be those that simply adopt new technology but those that connect, orchestrate, and operationalize it effectively.
The question is no longer build vs buy.
It is: How do you design a technology ecosystem that enables performance at scale?
Ready to Rethink Your Technology Strategy?
Incuvio helps health plans and provider organizations design and implement integrated, scalable technology ecosystems enabling risk adjustment performance, care gap closure, and operational efficiency.
Connect with our team to explore the right approach for your organization.